When a large-scale disaster strikes, a specialized unit of mental health experts, known as the Disaster Psychiatric Assistance Team (DPAT)*, enters and operates in the disaster area. After the Great East Japan Earthquake in 2011, Chiba University dispatched a mental health care team, and later in 2019, it created its own DPAT within the Chiba University Hospital. This DPAT subsequently became a part of the national DPAT.
The Division of Disaster Mental Health, Research Institute of Disaster Medicine, Chiba University is conducting research on the effects of disasters on the mind and the ways to deal with these effects based on emergency relief activities and clinical reality. One of the tools available to tackle the effects of disasters on the mind, is cognitive behavioral therapy. In this interview, we speak to Professor Masaomi Iyo, Head of the Division of Disaster Mental Health and Director of the Center for Forensic Mental Health, Chiba University, who is at the forefront of such activities in the field. We ask Professor Iyo about the significance of support for mental health in the event of a disaster and the prospects for research in the field.
*To support psychiatric care and mental health activities, a specialized team enters an area where a natural disaster, an aircraft or a train accident, a crime, or other mass disaster has occurred. Necessary care activities are performed in groups, with one group consisting of a psychiatrist, a hospital nurse, a public health nurse, an operations coordinator, and others. Within 48 hours of the disaster, advance teams are organized at each hospital to assess the needs of medical institutions in the affected areas. In case of a large-scale disaster, activity groups that are organized by prefectural governments rotate on a weekly basis or so for several weeks or months.
Supporting acute and chronic disaster responses from a mental health perspective

Please tell us about the activities through which you offer psychiatric support during disasters.
When a disaster or other emergency occurs, mental activity changes considerably over time, like a large wave.
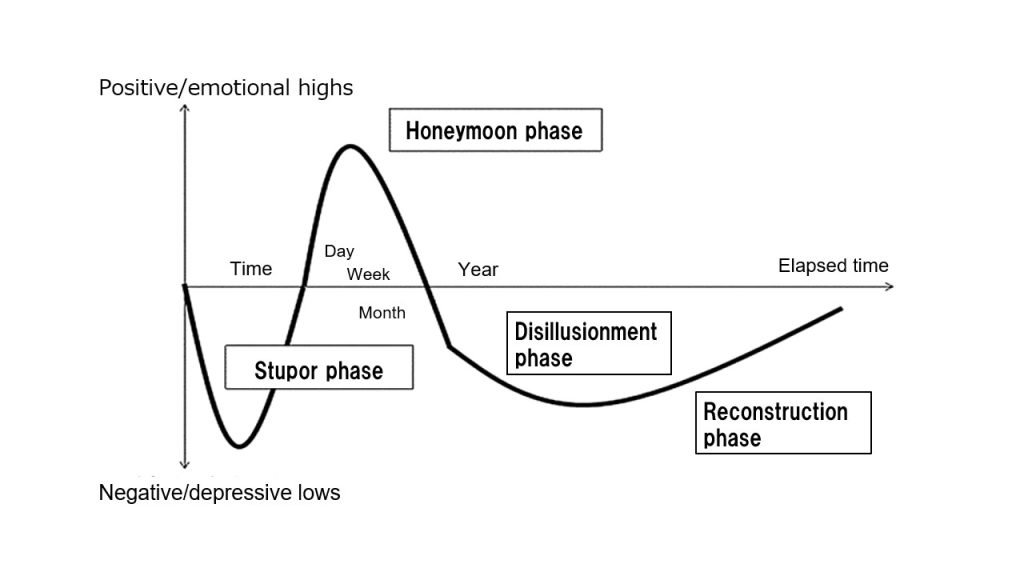
In the hyperacute and acute phases of disaster response that occur in the first few days after a disaster, survivors can experience acute stress and adjustment disorders, anxiety, psychosomatic disorders, worsening of pre-existing symptoms, grief reactions, and so on. While the needs specific to such disasters rapidly increase, medical institutions simultaneously face a considerable reduction in their capacity to conduct mental healthcare activities in the community. This is where DPAT comes into play—to support the local psychiatric care system and respond to the rapidly increasing psychological needs of disaster victims.
The damaging effects of large-scale disasters are long-lasting. What kind of medium- to long-term psychiatric support do you provide?
Areas affected by large-scale disasters have a honeymoon phase that is temporarily uplifting. To elaborate, initially, the disaster victims help each other and form bonds at evacuation centers and elsewhere, but the mood drops sharply with the onset of the chronic phase. Eventually, even seemingly healthy people are stressed from continued living in a deteriorating environment. This leads to depressive reactions, PTSD, alcoholism, suicide attempts, and so forth, as they enter what is called the disillusionment phase. Stress management is important at this point.
DPAT is aware of these mental health changes and helps local psychiatric care systems recover and return to their daily routines. After the Great East Japan Earthquake, Chiba University supported Higashimatsushima City, Miyagi Prefecture, for one year.
It’s not just natural disasters. During the infection spread phase of COVID-19, we provided psychiatric support to the passengers and crew aboard the Diamond Princess as well.
Mind, body, and reactions to an event are multiplied to generate action
Why do some people experience stress when others do not, even in similar situations?
Even if it is the same event, there are individual differences in how we react to hardships; the changes in emotions, the effects on the body, and the subsequent actions differ depending on the person. In other words, you could say that stress is a product of individual mental and physical states and the way that each person reacts to their situation.
Conversely, if we can change the way we see and perceive things, we will be more likely to be able to handle things calmly, even in an emergency such as a disaster.
What kind of mental changes happens when an infectious disease spreads?
When it comes to infectious diseases, you have anxiety about directly observable symptoms and anxiety about the infection spreading in places you cannot see and not knowing when you might be infected. What is important here is how to understand information, such as news reports and social media, that you will come across everywhere in society. In some cases, they can lead to actions that further spread the infection.
The results of a questionnaire survey on trends in Japan, Spain, and the United Kingdom show that information on the same virus, such as attitudes toward face masks, is perceived and acted on differently depending on the country. As the ways in which we receive and react to information become more diverse, the key question that arises may be, “How can we convey correct information to as many people as possible?” This is also true for stress caused by nuclear accidents and such.
The potential of disaster support through cognitive behavioral therapy

Controlling the way you look at things and your perceptions is important for dealing with stress, isn’t it?
Cognitive behavioral therapy is considered a highly effective form of psychotherapy for handling mental difficulties during a disaster. Chiba University has been incorporating cognitive behavioral therapy in earnest since 2000.
You need to know how to react to the event, understand the information necessary to deal with it appropriately, and apprehend emotional changes and behavior. By repeating this process, you will be able to acquire a multifaceted coping method that is tailored to meet your needs.
When it comes to preparing for a disaster emergency, there is the common dictum, “have the right kind of fear.”
Fear stops you from thinking. There is a saying that I often tell my patients, “Nothing ventured, nothing gained.” By taking a step forward, recognizing that you are in a whirlpool, and understanding your fears and anxiety, you will be able to float without being caught in the torrent. That is the starting point of cognitive behavioral therapy. If you undergo this kind of training in normal times, you will be able to control yourself when disaster suddenly strikes.
Medical care and drug discovery technology as tools for handling mental stress
What kind of collaboration can you expect from working with the Research Institute of Disaster Medicine?
Chiba University has two laboratories in the School of Medicine: The Department of Psychiatry and the Department of Cognitive Behavioral Physiology. The university hospital has the Department of Clinical Psychiatry, the Department of Clinical Child Psychiatry, and the Cognitive Behavioral Therapy Center. Finally, there are the university-affiliated centers that are the Center for Forensic Mental Health and the Research Center for Child Mental Development. So, there is a wealth of psychiatric care research and clinical practice. We also have extensive cooperation with departments that conduct drug discovery research. For example, the antidepressant fluvoxamine has been found to help prevent COVID-19 infections from becoming critical and has already entered the clinical trial stage.
By working with the Research Institute of Disaster Medicine, we are trying to accumulate knowledge about the common pillar of disaster response. This includes knowledge from medical fields like psychiatry and drug discovery, as well as knowledge from previously untapped research conducted by experts in information engineering and social sciences. I am looking forward to further developments.
Please tell us about the future prospects of your research.
We are particularly focused on children and education. The Department of Clinical Child Psychiatry at Chiba University has treated thousands of children, and I feel that the number has increased significantly in recent years.
When cornered, most children end up thinking that they have done something bad and are unable to ask for help. Learning how to deal with anxiety and stress from an early stage may reduce the difficulties of adolescents and younger adults.
Recently, for example, an educational program called Journey of the Brave (Yusha no Tabi) has been developed centered on the Research Center for Child Mental Development. Starting as elementary-school students, children undergo fun training and gradually become more robust through a repeated training process. It is important to train cognitive behavior as an extension of daily life this way.
We plan to continue disseminating information with various specialized fields, such as social education, collaboration with external organizations and companies, and contribute to society through mental health care.
Series
“Disaster Medicine” to Protect our Mind and Body from Disasters
The Research Institute of Disaster Medicine aims to build a disaster medicine and nursing system in the post-corona era. In addition to researchers of medicine, pharmacy, and nursing, those of horticulture, engineering, humanities, and sociology work together to create a new society.
-

#1
2022.10.25
Creating a Pandemic-Resilient Society to Tackle Future Invisible Enemies
-

#2
2022.12.07
Shedding Light on the Public Health Nurses Working at the Front Lines of Disaster-Stricken Areas
-

#3
2022.12.12
What causes nations and regions to perceive the COVID-19 crisis differently?〜Insights from the Humanities and Social Sciences Needed for Disaster Management Research
-

#4
2022.12.20
Let Community-Based Disaster Reconstruction take roots
-

#5
2023.02.23
The role of the Research Institute of Disaster Medicine (RIDM): The indispensable research hub for urban digital transformation
-

#6
2023.02.27
Affecting behavioral changes through a combination of mind and body: How can we calmly cope with stress in the event of a disaster?
Recommend
-

The Joy of Work and The Delight of Nurturing: From Social Farming to Universal Farms
2025.02.10
-

A Day in the Life of a Sports DoctorProfessionals behind the world’s most prominent sporting events
2023.04.13
-

The reciprocity of life: The interactive relationships between people, plants, and the environment
2023.05.19



